- Industries
Industries
- Functions
Functions
- Insights
Insights
- Careers
Careers
- About Us
- Healthcare
- By Omega Team

Every year, countless patients around the world find themselves on transplant waiting lists, holding on to hope as the clock ticks relentlessly forward. For many, that hope fades when a compatible donor organ never becomes available, revealing one of the most painful limitations of modern healthcare. Despite remarkable medical advances, the global shortage of donor organs continues to cost lives and strain families, hospitals, and healthcare systems alike. In response to this crisis, a quiet yet transformative revolution is taking shape at the crossroads of biology, engineering, and medicine: lab-grown organs. What once belonged purely to the realm of science fiction is now advancing toward clinical reality. By enabling the creation of organs tailored to a patient’s own cells, this innovation promises fewer immune rejections, faster access to transplants, and improved long-term outcomes. More than a technological breakthrough, lab-grown organs signal a shift toward a more ethical, sustainable, and humane future for transplant medicine, one where waiting lists shrink and life-saving care becomes a certainty rather than a gamble.
The Transplant Crisis: A System Under Pressure
Organ transplantation is one of medicine’s greatest achievements, yet it faces three persistent challenges:
Severe Organ Shortages: The demand for transplantable organs far exceeds the available supply, leaving millions of patients on waiting lists for years. Many deteriorate medically while waiting, reducing their chances of survival even if an organ becomes available. In countless cases, patients die before a suitable match is found, turning scarcity into a silent global health emergency. This imbalance places emotional, financial, and operational pressure on families, clinicians, and healthcare systems alike.
Immune Rejection: Even when a donor organ is successfully transplanted, the recipient’s immune system may recognize it as foreign and attack it. To prevent rejection, patients must take lifelong immunosuppressive medications. These drugs increase vulnerability to infections, cancers, and chronic conditions, often diminishing quality of life. Over time, immune complications can still lead to organ failure, necessitating repeat transplants or lifelong medical intervention.
Ethical and Logistical Barriers: Organ transplantation is constrained by complex ethical, legal, and logistical considerations. Donor availability depends on consent, cultural beliefs, and legal frameworks that vary widely across regions. Matching donors and recipients requires precise compatibility, rapid coordination, and advanced infrastructure. Inequities in access, along with risks of organ trafficking and exploitation, further complicate the system and raise serious moral concerns.
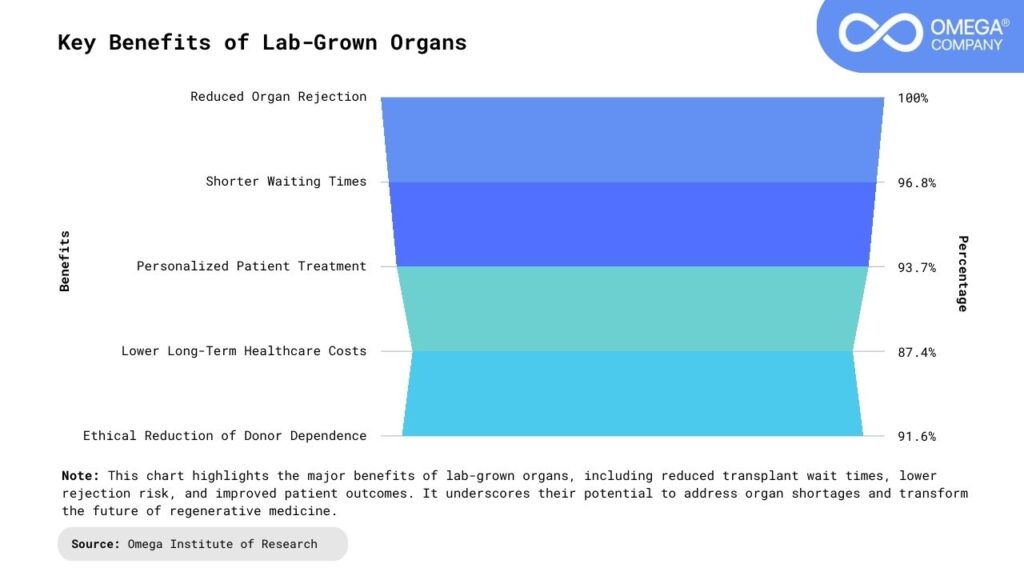
What Are Lab-Grown Organs?
Lab-grown organs also known as bioengineered or tissue-engineered organs—are created using a patient’s own cells, cultivated and structured into functional tissues or whole organs in a laboratory setting.
Stem Cells: Stem cells, often harvested from the patient, serve as the foundational building blocks of lab-grown organs. These cells have the unique ability to differentiate into various specialized cell types, such as heart, liver, or kidney cells. Because they originate from the patient’s own body, they offer a personalized solution that aligns with individual genetics. This not only improves compatibility but also reduces dependence on immunosuppressive drugs. Advances in stem cell science have made it possible to reprogram adult cells, expanding accessibility and ethical acceptability.
Scaffolds: Scaffolds act as the structural framework that gives a lab-grown organ its shape and architecture. Made from biodegradable materials or decellularized natural tissues, they provide physical support while guiding cells to grow in the correct patterns. As cells multiply and organize, the scaffold gradually dissolves or integrates into the developing tissue. This process mimics the body’s natural extracellular matrix, allowing organs to develop realistic form and function. Precision in scaffold design is crucial for ensuring proper blood flow, strength, and long-term performance.
Bioreactors: Bioreactors are highly controlled environments that simulate the conditions inside the human body. They regulate factors such as temperature, oxygen levels, nutrients, and mechanical forces to support healthy tissue growth. Within these systems, cells are “trained” to behave like they would inside a living organ. Bioreactors also allow scientists to monitor development in real time, improving consistency and safety. This controlled maturation process is essential for transforming clusters of cells into viable, transplant-ready organs.
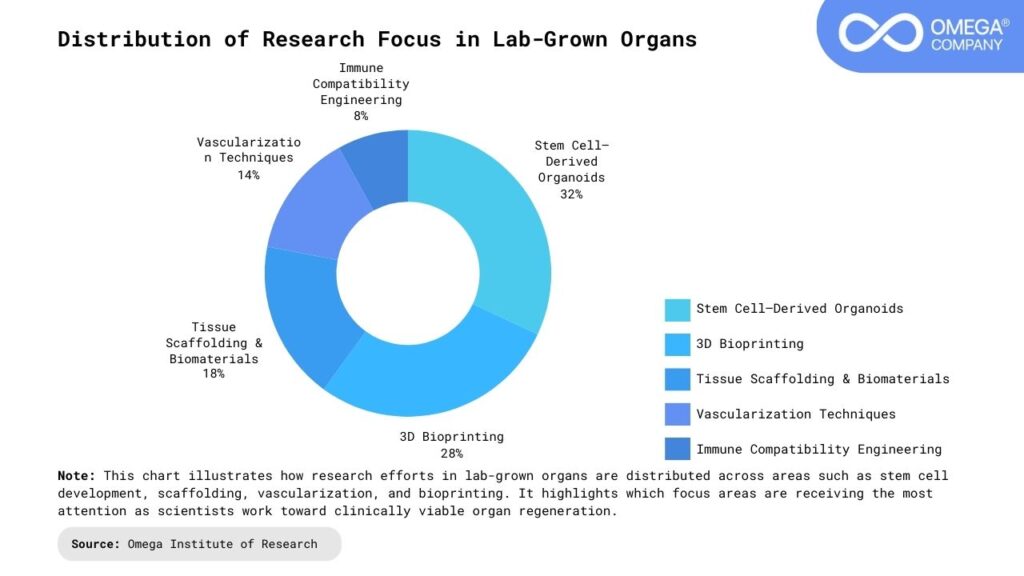
How Close Are We to Fully Functional Organs?
While fully lab-grown hearts or livers are still under development, major breakthroughs are already happening:
Lab-Grown Skin: Lab-grown skin is one of the most established and widely used applications of tissue engineering today. It is routinely applied in the treatment of severe burns, chronic wounds, and skin disorders. These engineered skin grafts help reduce infection risks, speed up healing, and minimize scarring. Because they can be produced in large quantities, they also ease pressure on donor skin availability. This success has paved the way for more complex tissue engineering efforts.
Bioengineered Bladders: Bladders grown from a patient’s own cells have already been successfully implanted in clinical trials. These organs are designed to integrate naturally with the body, reducing the likelihood of immune rejection. Patients receiving bioengineered bladders have shown improved organ function and quality of life. This milestone proves that lab-grown organs can survive, function, and adapt inside the human body. It represents a critical step toward engineering more complex organs.
Mini-Organs (Organoids): Organoids are tiny, simplified versions of organs such as kidneys, livers, and lungs grown in the laboratory. While too small for transplantation, they closely mimic real organ behavior at a cellular level. Researchers use organoids to study disease progression, test drug responses, and explore genetic disorders. This approach allows safer, faster, and more accurate experimentation than traditional methods. Organoids are also accelerating personalized medicine by predicting how individual patients might respond to treatments.
3D Bioprinting: 3D bioprinting has enabled scientists to precisely layer living cells into complex, functional structures. Using bio-inks made from cells and biomaterials, researchers have successfully printed blood vessels, cartilage, and bone tissue. These structures show promising integration and durability when implanted. Bioprinting allows for customization based on patient anatomy, improving surgical outcomes. As printing resolution and material science improve, this technology is expected to play a central role in building fully functional organs.
Why Lab-Grown Organs Are a Game-Changer
Personalized Medicine at Its Best: Because lab-grown organs are developed from a patient’s own cells, the risk of immune rejection drops dramatically. This approach aligns perfectly with the principles of personalized medicine, tailoring treatment to an individual’s unique biology. As a result, patients may no longer require lifelong immunosuppressive drugs. Reducing dependence on these medications also lowers the risk of infections, chronic complications, and long-term side effects. Ultimately, transplants could become safer, more predictable, and easier to manage over time.
Ending the Organ Shortage: Instead of relying on the limited availability of donor organs, hospitals could one day grow organs on demand. This shift would transform transplantation from a waiting-list lottery into a planned, timely medical procedure. Patients would receive treatment before their condition becomes critical, improving outcomes. Healthcare systems could better allocate resources and reduce emergency interventions. In the long run, this could save countless lives and reduce the emotional toll on patients and families.
Ethical Simplicity: Lab-grown organs bypass many of the ethical challenges associated with traditional organ donation. Issues such as donor consent, organ trafficking, and exploitation become far less relevant. This creates a more transparent and equitable medical pathway. Cultural and religious concerns around donation may also be minimized. By removing ethical ambiguity, trust in transplant systems can be significantly strengthened.
Better Outcomes, Longer Lives: Organs grown specifically for a patient are more likely to integrate seamlessly with the body. Improved compatibility enhances organ function and durability over time. Patients may experience faster recovery, fewer complications, and better long-term health. This leads to higher survival rates and an improved quality of life. In many cases, lab-grown organs could turn fatal conditions into manageable or curable ones.
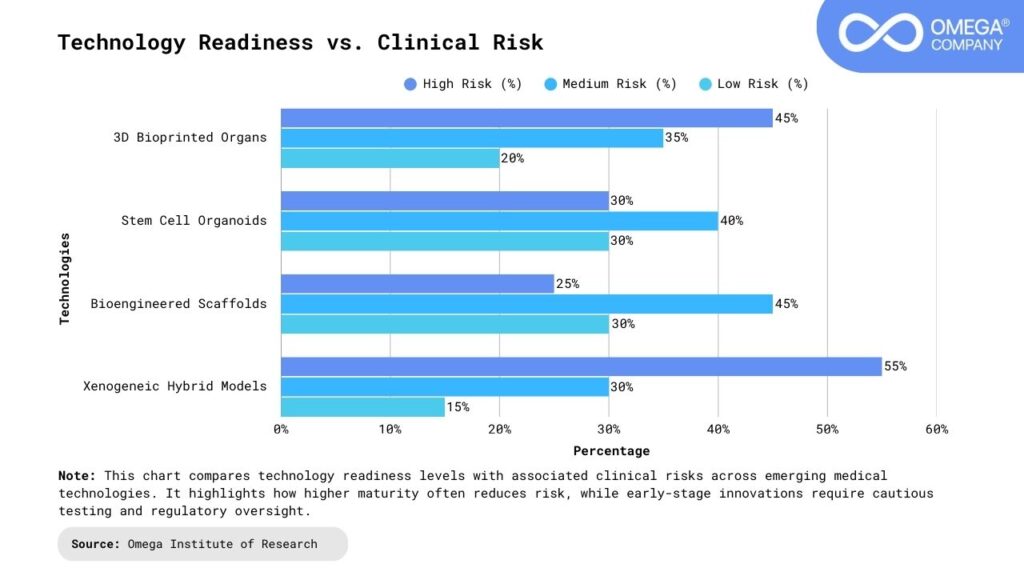
Beyond Transplants: Broader Medical Impact
The implications of lab-grown organs go far beyond transplantation:
Drug Testing on Human Tissue: Lab-grown tissues allow researchers to test drugs directly on human cells without exposing patients to unnecessary risks. This improves the accuracy of safety and effectiveness data compared to traditional laboratory models. Potential side effects can be identified earlier in the development process. Personalized tissue samples can also predict how different individuals may respond to the same drug. This leads to safer medications and more informed clinical trials.
Disease Modeling: Scientists can recreate diseases such as cancer, Alzheimer’s, and rare genetic disorders using lab-grown organ models. These models closely mimic how diseases develop and progress in the human body. Researchers can observe cellular changes in real time and test targeted interventions. This approach enables deeper understanding of complex conditions. It also accelerates the discovery of more precise and effective treatments.
Reduced Animal Testing: Lab-grown human tissues reduce reliance on animal testing, addressing long-standing ethical concerns in medical research. Human-based models often provide more relevant results than animal studies. This shift improves the reliability of experimental outcomes. It also helps researchers comply with stricter ethical and regulatory standards. Over time, this could redefine how preclinical research is conducted globally.
Faster Innovation Cycles: Using lab-grown organs shortens the time required to develop and validate new drugs and therapies. Researchers can rapidly test multiple compounds and refine approaches early in the process. This reduces development costs and failure rates in later-stage trials. Faster innovation means quicker access to life-saving treatments for patients. Ultimately, it enables a more agile and responsive healthcare ecosystem.
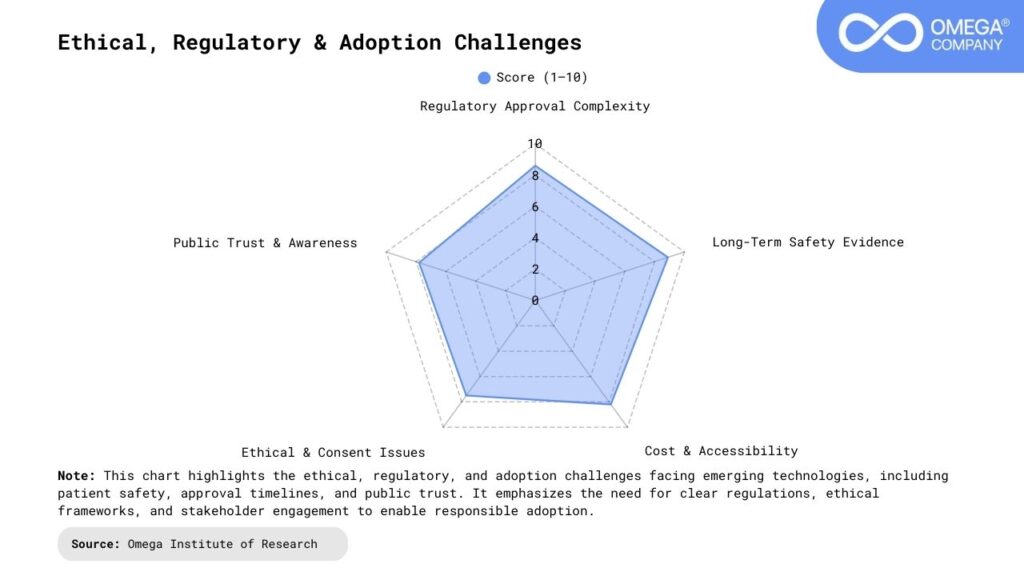
Conclusion
Lab-grown organs represent far more than a medical breakthrough; they mark a fundamental shift in how humanity approaches healing and recovery. By uniting stem cell science, bioengineering, and advanced manufacturing, transplant medicine is evolving from a system constrained by scarcity and uncertainty to one defined by personalization and possibility. As this technology continues to mature, it will not only save lives but also transform the entire experience of care, replacing prolonged waiting and risk with precision and reliability. Patients may receive organs designed specifically for their bodies, improving outcomes and restoring dignity to the healing process. In the broader story of modern medicine, lab-grown organs may be remembered as the moment when life-saving treatment moved from chance to choice ushering in an era where restoring health is faster, fairer, and fundamentally more human.
- https://healthcare-bulletin.co.uk/article/lab-grown-organs-the-future-of-rehabilitation-a-systematic-review-4407/
- https://www.labiotech.eu/in-depth/the-future-of-organ-transplants/
- https://imjhealth.org/organoids-and-lab-grown-organs-future-of-transplant-medicine
- https://www.longdom.org/open-access/the-future-of-artificial-organs-transforming-healthcare-with-bioengineering-1101863.html
- https://pmc.ncbi.nlm.nih.gov/articles/PMC10212693/
Subscribe
Select topics and stay current with our latest insights
- Functions